Clostridium tetani.pptx
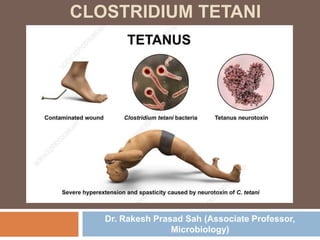
- 1. CLOSTRIDIUM TETANI Dr. Rakesh Prasad Sah (Associate Professor, Microbiology)
- 2. Clostridium tetani Causative agent of Tetanus Tetanus: an acute ds manifested by skeletal muscle spasm and autonomic nervous system disturbance. Known since ancient time; isolated by Kitasato (1889). Widely distributed in soil and intestine of man and animals. Ubiquitous
- 3. Morphology Gram positive Slender bacillus with spherical, terminal spores drumstick appearance Non-capsulated & motile (peritrichate flagella) Young cultures strongly Gram positive Old cultures even be Gram negative
- 4. Resistance Resistance of Cl. Tetani spores to heat vary in different strains. Most of the stains are killed by boiling for 10-15mins. Some resist boiling for 3 hrs. Autoclaving at 1210C for 20mins kills the spores of most strains. Spores are killed with Iodine (1% aqueous solution), H2O2 and Glutaraldehyde(2%) within few hours. Spores may survive in soil for years.
- 5. Toxins Produces two distinct toxins Tetanolysin (haemolysin) Tetanospasmin (neurotoxin)
- 6. Tetanolysin Heat and Oxygen labile
- 7. Tetanospasmin Proteinous in nature. Heat labile and oxygen stable. Powerful neurotoxin. Rapidly destroyed by proteolytic enzymes. Plasmid coded. Responsible for clinical manifestation of tetanus.
- 8. Tetanospasmin Lethal to mice and pigs in minute doses (0.0000001mg for mouse). Good Ag and is specifically neutralized by the antitoxin. Is plasmid coded. Can be toxoided by formaldehyde retains Ag property looses virulence property used for vaccine preparation.
- 10. Mechanism of Action of Tetanus Toxin Toxin binds to receptors (polysialogangliosides) present on motor nerve terminals which results in toxin internalization. After internalization, tetanus toxin gets transported in retrograde way to the gamma-aminobutyric acid (GABA) and glycine producing inhibitory neuron terminals Toxin prevents presynaptic release of inhibitory neurotransmitters glycine and GABA, which leads to spastic muscle contractions.
- 15. Pathogenesis Mode of transmission Injury (superficial abrasions, punctured wounds, RTA) Surgery done without proper asepsis. Neonates: Following abortion/delivery, due to unhygenic practices
- 16. Cl. Tetani has litte invasive power Tetanus develops following contamination of wounds with Cl. Tetani spores Source of infection may be soil, dust, faeces etc Infection remains localized in the wound Germination of spores and toxin production occur only if favorable condition exist
- 17. Pathogenic effects are due to tetanospasmin (neurotoxin) Acts presynaptically, Specifically blocks synaptic inhibition in the spinal cord Abolition of spinal inhibition leads to uncontrolled spread of impulses initiated anywhere in the central nervous system. Results in muscle rigidity and spasms due to the simultaneous contraction of agonists and antagonists.
- 18. Clinical Manifestations I.P. 6-10 days. Muscles of the face and Jaw are affected first (due to shorter distances for the toxin to reach the pre-synaptic terminals). First symptoms Increase in the masseter tone leading to trismus or lockjaw, followed by muscle pain and stiffness, back pain and difficulty in
- 19. Clinical Manifestations Neonates difficulty in feeding (initial presentation) Ds progression Painful mscle spasm Localised (affected limb) Generalized (descending spastic paralysis)
- 20. Risus sardonicus Abnormal, sustained spasm of facial muscles produces grinning.
- 21. Opistotonos position Abnormal posture of body (due to generalized spastic contraction of the extensor muscles) Respiratory muscles spasm airway obstruction.
- 23. Autonomic disturbances (max 2nd week) Severe tetanus Low or high blood pressure Tachycardia Intestinal stasis Sweating Increased tracheal secretions Acute renal failure
- 24. Laboratory Diagnosis Specimen Wound swab Exudate or tissue from the wound. Gram Staining GPB with terminal and round spores (drum stick appearance). But indistinguishable C. tetani from morphologically similar to C. tetanomorphum and C. sphenoides.
- 25. Laboratory Diagnosis Culture RCM Meat particle black Blood agar with polymyxin B Swarming growth BCP and C CT
- 26. Prophylaxis Surgical Removal of foreign body, blood clots to prevent anaerobic condtions. Antibiotics Penicillin Erythromycin Immunisation Active immunisation Passive immunisation Combined prophylaxis
- 27. Active immunisation Most effective method Tetanus toxoid (formal toxoid) Dose:- 0.5ml I.M. TT(Tetanus toxoid) is given with DPT in children DPT:- 6,10,14 weeks of birth. DPT:-Booster dose 16-24 weeks and 5years. TT:- Additional 2 doses of TT at 10 and 16 years. For prevention of Neonatal tetanus, all pregnant women are given 2 doses of TT at
- 28. Passive Immunisation Antitetanus serum (ATS) prepared by immunising horse with toxoid for preventing tetanus. Human antitetanus immunoglobulins (HTIG).
- 29. Combined Prophylaxis In non-immune person Tetanus toxoid ATS or HTIG
- 30. Thank You...
